Biological Dentistry and Chronic Illness: The Missing Link Most People Never Consider
Dental amalgams and mercury exposure are rarely discussed in chronic illness recovery. Learn how biological dentistry connects to inflammation, toxic burden, and whole-person health — and why it may be the missing piece in your recovery.
DETOXIFICATION AND MERCURY BURDEN
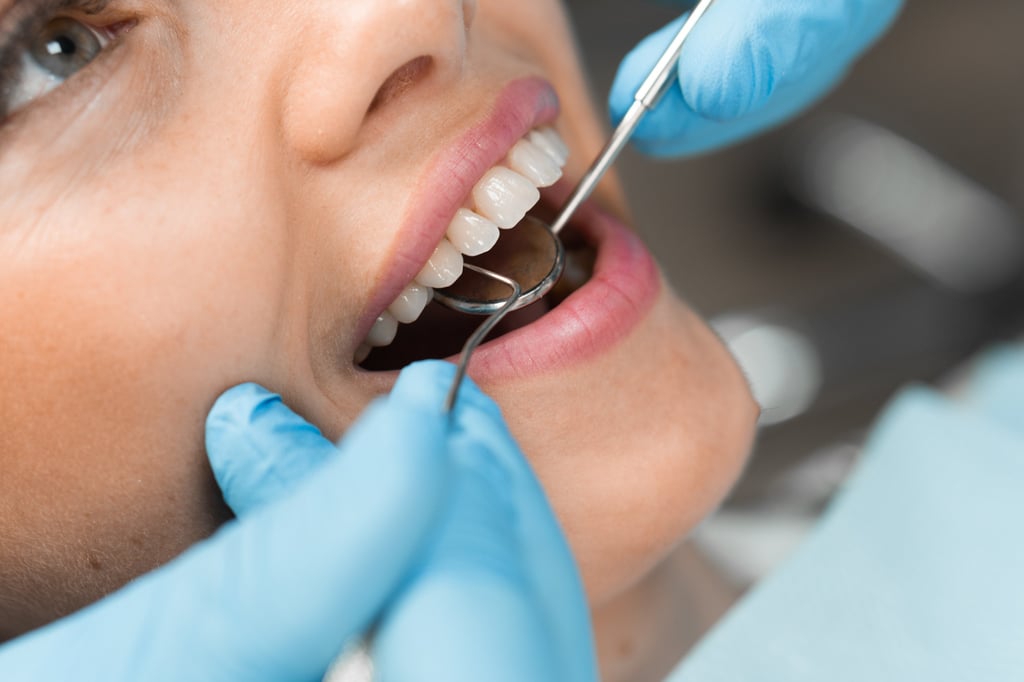
When people begin exploring integrative approaches to chronic illness, they typically focus on diet, gut health, inflammation, detoxification, and stress. These are all genuinely important areas — and addressing them thoughtfully produces real results for many people.
But there is one dimension of health that rarely enters the conversation, even in integrative contexts, and that for a significant subset of people represents one of the most meaningful and overlooked contributors to their chronic burden: the mouth.
Biological dentistry — sometimes called holistic or biocompatible dentistry — is a field of dental practice that considers the impact of dental materials, procedures, and oral health on the body as a whole. It is not a fringe concept. It is grounded in well-documented physiology and growing research, and it addresses a dimension of toxic and inflammatory burden that conventional medicine and most integrative health approaches simply do not evaluate.
For people who have done significant work on their health — improved their diet, supported their gut, addressed inflammation — and still find themselves plateauing without explanation, the dental dimension may be the missing piece.
What Is Biological Dentistry?
Biological dentistry approaches oral health through the lens of whole-body impact. It asks not only whether a dental procedure is technically successful, but whether the materials used and the biological effects produced are compatible with the patient's overall health.
This includes attention to the biocompatibility of dental materials — which metals, resins, and compounds are used in fillings, crowns, implants, and other restorations — as well as the systemic implications of dental infections, root canals, cavitations, and the structural relationship between the jaw, teeth, and the broader nervous and lymphatic systems.
The central concern of biological dentistry that is most relevant to chronic illness recovery is amalgam — the silver-colored filling material that has been used in dentistry for over 150 years and that contains approximately fifty percent mercury by weight.
What Are Dental Amalgams and Why Do They Matter?
Dental amalgam is an alloy composed primarily of mercury, silver, tin, and copper. It has been widely used as a restorative material because of its durability, ease of application, and low cost. For most of the twentieth century, it was considered safe and stable once placed — the assumption being that mercury in amalgam was bound and inert.
That assumption has been significantly revised by subsequent research.
Mercury vapor release is continuous and measurable. Modern research has established clearly that dental amalgam fillings release mercury vapor continuously — not only during placement and removal, but throughout their lifespan. Activities that increase chewing pressure, heat, or abrasion — eating, drinking hot beverages, teeth grinding, and even brushing — increase the rate of vapor release. The mercury vapor released is inhaled and absorbed through the lungs with high efficiency, entering the bloodstream and distributing to tissues throughout the body.
The nervous system and kidneys are primary accumulation sites. Mercury has a particular affinity for nervous system tissue and the kidneys. Once absorbed, inorganic mercury from amalgam is converted in tissues to organic methyl mercury, which crosses the blood-brain barrier and accumulates in neural tissue. This accumulation is gradual and silent — it does not produce acute poisoning symptoms in most people, but contributes to a chronic background burden that affects neurological function, immune regulation, and inflammatory activity over time.
Individual variation in mercury handling is significant. Not everyone with amalgam fillings develops significant mercury burden. Genetic variation in the enzymes responsible for mercury metabolism and excretion — particularly those involved in glutathione production and methylation — means that some individuals accumulate mercury far more readily than others at equivalent exposure levels. This explains why two people with similar numbers of amalgam fillings can have very different health outcomes — and why mercury burden is not always predictable from the number of fillings alone.
The immune system response to mercury is real and varied. Mercury is a potent immunotoxin. It can directly activate immune cells, trigger autoimmune responses in susceptible individuals, and contribute to the kind of chronic immune dysregulation that underlies many chronic inflammatory conditions. For people with autoimmune tendencies or significant immune reactivity, amalgam exposure may represent a relevant ongoing trigger.
How Does Dental Mercury Connect to Chronic Illness?
The connection between dental mercury and chronic illness is not a simple cause-and-effect relationship. Mercury from amalgam is one contributor among many to the body's total toxic and inflammatory burden — and its significance varies considerably between individuals depending on their genetic profile, detoxification capacity, number and age of fillings, and overall health status.
What research and clinical observation consistently suggest, however, is that for a subset of people with chronic illness — particularly those with neurological symptoms, immune dysregulation, autoimmune conditions, unexplained fatigue, and symptoms that have not responded to other interventions — dental mercury represents a clinically relevant burden that deserves evaluation.
Neurological and cognitive symptoms. Brain fog, memory difficulty, reduced cognitive clarity, mood disturbances, and neurological sensitivity are among the symptoms most consistently associated with mercury accumulation. Because mercury has a particular affinity for neural tissue, its effects on the nervous system are often more pronounced than its effects on other organ systems.
Immune dysregulation and autoimmunity. Mercury's immunotoxic properties make it a relevant consideration for people with autoimmune conditions, chronic allergic reactivity, and immune dysregulation. It can act as a hapten — binding to proteins and making them appear foreign to the immune system — triggering immune responses that can become self-perpetuating even after the original trigger is addressed.
Chronic fatigue and mitochondrial burden. Mercury interferes with mitochondrial function — disrupting the cellular energy production pathways that are already compromised in many people with chronic fatigue. This connection helps explain why some individuals with significant amalgam burden experience fatigue that is disproportionate to their other identifiable health factors.
Kidney burden. The kidneys are a primary route of mercury excretion and a primary site of accumulation. Chronic mercury exposure from amalgam places a sustained burden on renal function that can impair the kidneys' capacity to filter and eliminate other toxins — contributing to a broader pattern of impaired detoxification.
Hormonal disruption. Mercury has been shown to interfere with thyroid hormone metabolism and to disrupt the body's hormonal signaling in ways that contribute to fatigue, mood disturbances, and metabolic dysregulation — areas that overlap significantly with the presentation of many chronic illness conditions.
Why Is This Dimension So Rarely Discussed?
The relative absence of dental mercury from mainstream chronic illness conversations reflects several overlapping factors.
Dentistry and medicine operate as separate disciplines with limited cross-communication. A physician evaluating chronic fatigue or autoimmune disease rarely inquires about dental history, and a conventional dentist rarely considers the systemic health implications of the materials they place. The result is a significant gap in the evaluation of chronic illness that integrative approaches are only beginning to address systematically.
The regulatory status of amalgam has also contributed to confusion. While regulatory agencies in many countries have maintained that amalgam is safe for most people — based primarily on average population exposure rather than individual susceptibility — the scientific literature on mercury's biological effects is substantially more nuanced. Several countries have restricted or phased out amalgam use, and awareness of the issue continues to grow among both practitioners and patients.
It is worth noting that major regulatory bodies including the FDA and WHO consider amalgam safe for the general population. The concern addressed in integrative health contexts relates primarily to individuals with heightened susceptibility — genetic, immunological, or otherwise — for whom individual evaluation may be more relevant than population-level conclusions.
Finally, the gradual and systemic nature of mercury accumulation makes it difficult to connect to specific symptoms in any straightforward way. Without targeted evaluation — which standard medical testing does not provide — mercury burden remains invisible, and its contribution to chronic illness goes unrecognized.
What Does Evaluation and Support Look Like?
For people who suspect that dental mercury may be a relevant factor in their chronic illness, evaluation and support require a careful and informed approach.
Working with a biological dentist. A biological or biocompatible dentist can evaluate the number, age, and condition of existing amalgam fillings, assess overall oral health from a whole-body perspective, and — where amalgam removal is indicated — apply safe removal protocols that minimize mercury vapor exposure during the procedure. Safe amalgam removal is significantly different from standard removal, and the distinction matters considerably for how much additional mercury burden the person is exposed to during the process.
Timing and preparation matter. Amalgam removal in the context of chronic illness is not a simple intervention. For people with significant mercury burden, impaired detoxification capacity, or active immune dysregulation, removal without adequate preparation and support can temporarily increase symptoms. Working with both a biological dentist and an integrative health practitioner to prepare the body's detoxification pathways before and support them through and after removal is an important part of ensuring that the process supports rather than burdens recovery.
Mercury burden evaluation. Standard blood mercury levels reflect recent exposure rather than tissue accumulation, and are often within normal range even in people with significant chronic burden. More informative approaches to evaluation include provoked urine testing and other functional assessments — always interpreted in the context of the individual's full clinical picture rather than in isolation.
Integration with the broader recovery process. Addressing the dental dimension is most effective when it is integrated with the broader recovery process — including gut support, nutritional optimization, and detoxification support — rather than pursued in isolation. The body's capacity to process and eliminate mercury released during removal depends on the same pathways that support general detoxification, and those pathways need to be functioning well for the process to proceed safely and effectively.
A Dimension Worth Knowing About
Biological dentistry and dental mercury are not relevant for every person navigating chronic illness. But for those who have done significant recovery work and continue to plateau — or who recognize patterns of neurological, immune, or fatigue-related symptoms that have never been fully explained — the dental dimension deserves serious consideration.
Understanding that the mouth is not separate from the body, and that the materials placed in it have biological effects that extend far beyond the teeth, is a foundational shift in perspective that opens a dimension of recovery support that most people have never been offered.
Explore Whether This Program Is Right for You
If you are navigating chronic illness and are looking for a recovery process that considers the whole person — including dimensions like dental burden that are rarely addressed elsewhere — the BLIRM Method may offer the kind of comprehensive, thoughtful support you have been looking for.
The information in this article is educational in nature and is not intended as medical advice. BLIRM-Method is an integrative support program and does not replace the care of licensed healthcare providers.
Fanny Barquero
Guided Integrative Recovery Support
© 2026 Fanny Barquero. All rights reserved.
